Tonsils and adenoids
The tonsils
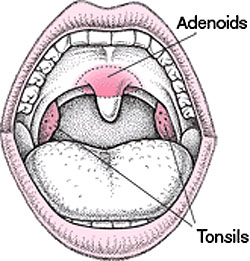
The tonsils are two clumps of tissue, on either side of the throat, embedded in a pocket at the side of the palate (roof of the mouth) – the lower edge of each tonsil is beside the tongue – way in the back of the throat. Each tonsil has pits on its surface (crypts) that go into the tonsil. During eating and drinking the tonsils are pushed together by the throat muscles and small particles of food may lodge in the tonsil crypts – potentially leading to infection.
The adenoid
The adenoid is a single clump of tissue in the back of the nose (nasopharynx). They are located on the back wall of the throat (pharynx) about two centimetres above the uvula (the little teardrop shaped piece of tissue that hangs down in the middle of the soft palate).
What function do the tonsils and adenoids serve – are they important?
- The tonsils and adenoid are mostly composed of lymphoid tissue, which is found throughout the gastointestinal tract and on the base of the tongue
- Lymphoid tissue is composed of lymphocytes which are mostly involved in antibody production – since we generally consider antibody production to be a good thing, many studies have been performed to try to clarify the importance of the tonsils, and there seems to be no adverse effect on the immune status or health of patients who have had them removed
- Any noticeable effect has generally been positive and it appears that the tonsils and adenoids do not effectively handle the huge number of viral infections that occur in children in an urban population – the immune system, including the tonsils and adenoids, developed during a era where the child was rarely exposed to a large number of other people and the germs they carried
- It may also be that the tonsils and adenoids are relatively more important in dealing with certain types of infections, such as worms or other parasites that are relatively uncommon in today’s society
- It is clear that the immune system may improve after diseased tonsils and adenoids are removed
Adenoid removal – when is surgery necessary?
If an enlarged or infected adenoid keeps bothering your child and are not controlled by medication, the doctor may recommend surgically removing them with an adenoidectomy.
This may be recommended if your child has one or more of the following:
- Blocked nose
- Recurrent infections
- Ear infections, middle ear fluid, and hearing loss requiring a second or third set of ear tubes
Having your child’s adenoids removed is especially important when repeated infections lead to sinus and ear infections. Severely swollen adenoids can interfere with middle ear function and hearing – this can sometimes lead to infections or middle ear fluid causing a temporary hearing loss. Children with infected adenoids may have sore ears and ear pain – those children with glue ear might also need an adenoidectomy at the time of their ear tube surgery. Even though some children need surgery, remember that enlarged adenoids are normal in others.
If your child’s adenoids aren’t infected, your doctor may choose to wait to operate because the adenoids may eventually shrink on their own as adolescence approaches.
Tonsils and adenoid removal – when is surgery necessary?
There are a number of well-established valid reasons for removal – some patients will have more the one reason.
The most common reasons to remove the tonsils / adenoids include:
- Snoring in Children
- Blockage of the nose and throat – they are too big
- Chronic and recurrent tonsillitis – sore throats
- White debris in the tonsils – bad breath
- Unusual enlargement or appearance – as a biopsy for suspected tumour
Snoring in children
- Sleep disordered breathing in children is often caused by enlargement of the tonsils and adenoids
- The child sleeps with the mouth open and the head bent back and snores – often the child’s breathing has stops or pauses followed by snorting
- Other symptoms include bedwetting, slow growth, headache, irritability, poor concentration and misbehaviour
- Big tonsils can also cause difficulty with eating and drinking in children
- Sleep disordered breathing caused by enlargement of the tonsils and adenoids is an indication for surgery
Click here for more information about snoring in children.
The tonsils and tonsillitis
Tonsillitis is an inflammation of the tonsils in the mouth and will often cause a sore throat and fever – the adenoids are often infected at the same time. Symptoms may also include a sore throat, difficulty with eating and drinking and loss of appetite, bad breath, fever, swollen neck glands, and generally feeling irritable and unwell.
During episodes of tonsillitis the tonsils will become swollen and red often with debris on the surface. Most people get tonsillitis at some time – it is common for children to get repeated episodes of tonsillitis with associated tonsil thickening and scarring.
Chronic tonsillitis
- After repeated acute infections or low-grade infection, chronic tonsillitis can develop
- The tonsils become scarred and trap bacteria and debris within the crypts
- Symptoms persist despite treatment with antibiotics
Types of tonsillitis
There are 3 main types of tonsillitis: acute, subacute and chronic.
- Acute tonsillitis can either be bacterial or viral in origin
- Subacute tonsillitis (which can last between 3 weeks and 3 months) is caused by the bacterium Actinomyces
- Chronic tonsillitis, which can last for long periods if not treated, is almost always bacterial, and is extremely painful
Tonsillitis causes
Bacterial tonsillitis may be caused by Group A streptococcal bacteria, resulting in strep throat. Viral tonsillitis may be caused by numerous viruses such as the Epstein-Barr virus (the cause of glandular fever) or the Coxsackie virus. Sometimes, tonsillitis is caused by a superinfection of spirochaeta and treponema, in this case called Vincent’s angina.
Tonsillitis medical treatment
Treatment consists of painkillers and fluids; if caused by bacteria then antibiotics are also prescribed – usually penicillin, or erythromycin if the patient is allergic to penicillin. Amoxicillin should not be used, unless bacterial infection has been microbiologically confirmed, because if mononucleosis is mistaken as tonsillitis and amoxicillin is given, a rash might develop and it may be wrongly assumed that the patient has developed an allergy to penicillin. Rest in a warm environment is advisable.
Pain relief for tonsillitis
In many cases of tonsillitis, the pain caused by the inflamed tonsils warrants the prescription of topical anaesthetics for temporary relief – Viscous lignocaine (xylocaine) solutions are often prescribed for this purpose.
One may consider a burst of steroids to help decrease the swelling and inflammation thereby easing pain and allowing the patient to drink liquids sooner.
Duration of tonsillitis
When tonsillitis is caused by a virus, the length of illness depends on which virus is involved. Usually, a complete recovery is made within one week, however some rare infections may last for up to two weeks.
Glandular fever
Tonsillitis due to glandular fever (Epstein-Barr virus) often occurs in teenagers and can be severe with huge tonsil and adenoid swelling. The neck glands are also swollen. Partial blockage of the throat can develop leading to problems breathing, eating and drinking.
Complications of tonsillitis
Quinsy
- An abscess may develop lateral to the tonsil during an infection, typically several days after the onset of tonsillitis – this is termed a peritonsillar abscess (or quinsy)
- Rarely the infection may spread beyond the tonsil resulting in inflammation and infection of the internal jugular vein giving rise to a spreading septicaemia infection (Lemierre’s syndrome)
Chronic tonsillitis
- In chronic/recurrent cases (generally defined as seven episodes of tonsillitis in the preceding year, five episodes in each of the preceding two years or three episodes in each of the preceding three years), or in acute cases where the palatine tonsils become so swollen that swallowing is impaired, a tonsillectomy can be performed to remove the tonsils
- Patients whose tonsils have been removed are certainly still protected from infection by the rest of their immune system
Bad breath
- Bacteria which accumulates in pits (referred to as ‘crypts’) in the tonsils, produce whitish-yellow deposits known as a tonsilloliths – these ” tonsil stones ” emit a very pungent odour due to the presence of volatile sulphur compounds causing bad breath
- Tonsilloliths ( tonsil stones ) which occur in the crypts of the tonsils can only be completely cured by tonsillectomy
Snoring
- Hypertrophy of the tonsils can result in snoring, mouth breathing, disturbed sleep, and obstructive sleep apnoea, during which the patient stops breathing and experiences a drop in the oxygen content in the bloodstream
- A tonsillectomy can be curative when tonsil enlargement is the cause of airways obstruction
Joint and kidney complications
- In very rare cases, diseases like rheumatic fever or glomerulonephritis can occur
- These complications are rare in developed nations but remain a significant problem in poorer areas
- Click here for more information about tonsillitis and Rheumatic Fever
Surgical removal of the tonsils and adenoid (adenotonsillectomy)
Adenotonsillectomy is the most common children’s ENT operation. The tonsils and adenoid are removed from their sockets and in most cases can be removed with very little bleeding.
What happens during tonsils and adenoid removal
Surgery, no matter how common or simple the procedure, can be cause for concern for both children and parents.
You can help prepare your child for surgery by talking about what to expect:
- Your child will receive general anesthesia – this means the surgery will be performed in an operating room so that an anaesthetist can monitor your child
- Your child will be asleep for about 20 minutes
- The surgeon can get to the adenoid and tonsils with no need to cut through skin
- The adenoid and tonsils are removed and then the blood vessels are cauterized (sealed)
- Your child will wake up in the recovery area
- Children need to stay overnight for observation after surgery
What happens after removal of the tonsils and adenoid?
The typical recuperation after removal of the tonsils and adenoid often involves several days of moderate pain and discomfort. In less than a week or two after surgery, everything should return to normal. The throat will heal naturally, which means there are no stitches to worry about. There’s a small chance any tissue that’s left behind can swell, but it rarely causes new problems. After surgery, a child’s symptoms usually disappear immediately, unless there’s a lot of swelling that could lead to some temporary symptoms.
Recovery after child tonsil and adenoid removal
Normal findings
A white or yellow membrane will form on the throat where the tonsils were removed – this is normal healing tissue and will clear after 5 to 10 days.
Mouth care

- Brush your teeth at least 3 times per day
- Gargle with salt water and drink water as much as possible
- Chew gum as this creates saliva and helps with the healing process
Diet
- It is very important to re-establish eating and drinking as soon as possible – the longer the delay before eating and drinking the more discomfort there will be
- Drink plenty of fluid and chew gum to keep the throat moist
- Fluids are essential – start with ice chips, sips of water or your favourite juice drink, and progress to at least a 250mL glass of drink
- Cold liquids, non-acidic juices, ice cream and ice blocks are tolerated better in the first 24-hours after tonsillectomy
- Progress to soft foods gradually
- Avoid acid foods and juices, salty and fried foods and very hot food and drinks for two weeks
Click here for more information about what to eat after a tonsillectomy and adenoidectomy.
Bleeding
Bleeding after leaving hospital is uncommon. If bleeding is going to occur it would usually be within the first 14 days after surgery. Persistent spitting or vomiting blood is abnormal – notify you doctor. If you experience bleeding go straight to your nearest Emergency Department. Gargling with cold water or with 1% hydrogen peroxide may help bring bleeding under control.
Pain
A sore throat after tonsillectomy is common and will limit chewing – you may also experience referred ear pain. It is not unusual for your throat to become more painful on the 4th or 5th day after the operation. A good pain relief is to eat or drink and chew more – cooler foods may be soothing, for example, cold drinks and ice cream – chewing gum is also soothing. Take pain medication as prescribed every 4 to 6 hours as needed – Do not take aspirin, aspirin products or NSAIDs like Nurofen for pain relief as this may increase the risk of bleeding. Eating and drinking will be easier around 30 minutes after taking pain medication.
Activity
- Rest with limited activity at home for 24 – 48 hours after tonsillectomy
- Avoid lifting, straining or strenuous exercise for 2 weeks to prevent bleeding
Follow-up
Generally your follow-up will consist of:
- A visit six weeks after surgery – you will need to ring the office to make that appointment
- Review by your local doctor as needed
Country patients
If you are unable to return to Sydney for follow-up, it may be for your follow-up to be undertaken by your local doctor – we would need to confirm these arrangements before you leave hospital.
If you have questions about children’s tonsils and adenoid removal contact your local doctor, who will arrange for you to see an ear nose throat specialist.




