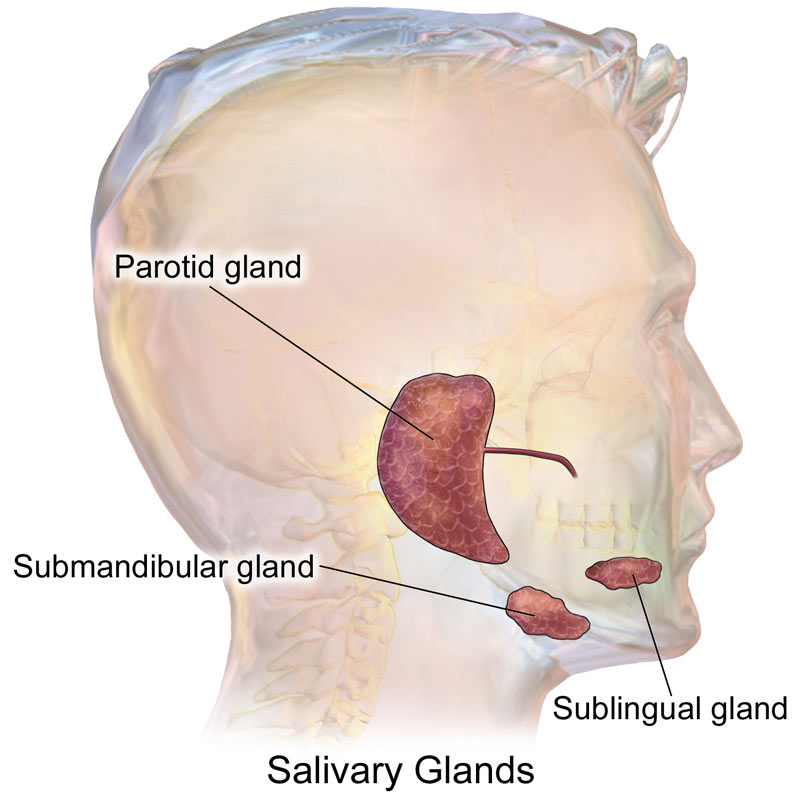
Submandibular Gland
Diagnosis and gland-preserving minimally invasive therapy for wharton’s duct stenoses
Michael Koch MD, Heinrich Iro MD, Julian Künzel MD, Georgios Psychogios MD, Alessandro Bozzato MD, Johannes Zenk MD, Laryngoscope, Article first published online: 9 DEC 2011
Objectives/Hypothesis:
The management of stenoses of Wharton’s duct has so far been little investigated or systematized. The development of minimally invasive treatment methods, including sialendoscopy, has made preservation of gland function possible.
Study Design
Retrospective study in a tertiary referral center.
Methods
A total of 153 stenoses of the submandibular duct were diagnosed and treated in 138 patients. Ultrasound and sialendoscopy were the first-choice diagnostic measures. A total of 62.7% of the stenoses were located in the distal, 11.1% in the middle segment, and 18.3% in the proximal to posthilar duct. Diffuse stenoses were observed in 7.8% of the cases. Sialendoscopy-assisted intraductal cortisone administration, interventional sialendoscopy, and transoral ductal surgery were the treatment options. The mean period between treatment and data collection was 52.5 months.
Results
Fibrotic stenoses were diagnosed in 88.3% and bilateral involvement in 8.6% of the cases. Distal stenoses were treated predominantly by ductal incision (79.2%). Stenoses of the midsubmandibular duct were treated conservatively in 29.4% or with sialendoscopy or ductal incision in 35.3% of cases each. Proximal up to posthilar stenoses could be dilated by interventional sialendoscopy in 82.2%. In 25% of all diffuse stenoses, glandular resection was carried out, representing 2.6% of all stenoses. Glandular function was preserved in 97.8% of cases.
Conclusions
Stenoses of the submandibular duct can be treated using minimally invasive procedures and with preservation of glandular function with a high success rate. Ductal incision procedures are the most important measure, but sialendoscopy becomes more important the more centrally the stenosis is located.
Reference
For more information
Click here for more information about the salivary glands.



